2026 Update from a UK-trained gastroenterologist in Dubai.
Introduction
One of my patients here in Dubai recently asked me about fecal microbiota transplant (FMT) for Crohn’s disease and ulcerative colitis, and I’ve also received many messages about it.
This is timely because FMT and the gut microbiome in inflammatory bowel disease (IBD) were discussed again at the recent Crohn’s & Colitis Congress in Las Vegas.
In this article, I’ll explain what FMT is, what current research suggests, why ulcerative colitis and Crohn’s disease can behave differently, what guidelines say, and why the microbiome still matters in IBD.
What Is Fecal Microbiota Transplant (FMT)?
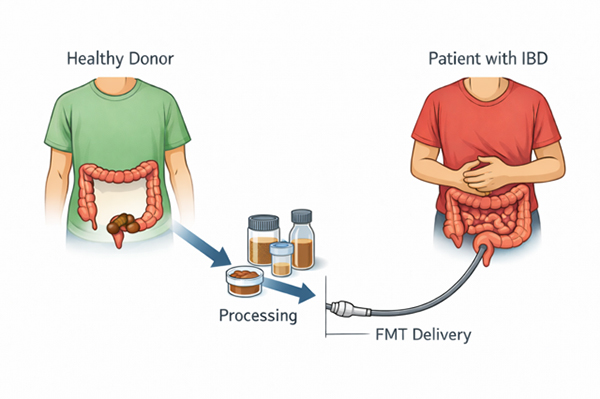
FMT involves transferring processed stool from a carefully screened healthy donor into the colon of a person with inflammatory bowel disease.
The aim is to influence the gut microbiome — the community of bacteria in the colon — which can affect inflammation in both Crohn’s disease and ulcerative colitis.
What Does the Latest Research Suggest?
Recent pooled research discussed at international IBD meetings suggests that adding FMT to standard therapy can produce a small but meaningful improvement in remission rates for ulcerative colitis.
For Crohn’s disease, results have been more mixed and less consistent, which is why the overall message remains more cautious.
In practice, the key point is that the effect is not dramatic, and outcomes vary — but the repeated finding that microbiome change can influence disease activity is scientifically important.
What Do International Guidelines Say?
Major international organisations (including leading US and European gastroenterology bodies) do not currently recommend FMT as routine treatment for Crohn’s disease or ulcerative colitis outside specialist or research settings.
FMT is established for recurrent Clostridioides difficile infection, but it is not considered standard therapy for inflammatory bowel disease at present.
Why Does the Microbiome Still Matter in IBD?
Even though FMT is not routine therapy, research consistently reinforces a core point: the gut microbiome plays a central role in inflammatory bowel disease, particularly ulcerative colitis.
Patients with IBD often have reduced microbial diversity, depletion of protective bacteria, and altered immune signalling influenced by microbial metabolites. This is why modern IBD research is increasingly focused on microbiome profiling and targeted microbiome-based approaches.
If you would like to learn more about the microbiome in Crohn’s disease and ulcerative colitis, please read:
Gut Microbiome in Crohn’s & Ulcerative Colitis (Dubai)
Frequently Asked Questions
What is fecal microbiota transplant (FMT)?
FMT involves transferring processed stool from a carefully screened healthy donor into the colon to influence the gut microbiome and potentially affect inflammation in IBD.
Does FMT work for ulcerative colitis and Crohn’s disease?
Signals are more consistent in ulcerative colitis than Crohn’s disease. Even in ulcerative colitis, overall benefit appears modest and varies between individuals.
Is FMT a standard treatment for IBD in Dubai?
No. International guidance does not currently recommend FMT as routine IBD treatment outside specialist or research settings, and it should not replace guideline-based therapy.
Recommended Guides
Ulcerative Colitis Basics & Patient Education
- AI in Crohn’s and Ulcerative Colitis: Can Machine Learning Predict IBD Treatment Response?
- MH002 next generation probiotic for ulcerative colitis
- Engineered Probiotic for Ulcerative Colitis 2026
- Gut Microbiome in Crohn’s Disease & Ulcerative Colitis
- Predicting Biologic Treatment Success in Crohn’s & Ulcerative Colitis
- Ulcerative Colitis Progression in Dubai: What the Research Shows + 3 Ways to Reduce Risk
- Don’t Ignore Your 5-ASA — Proven Treatment for Ulcerative Colitis
- Learn about Biologicals used in UC and Crohn’s in Dubai
- Biologics and Pregnancy
- Probiotics for Ulcerative Colitis: What Actually Works?
- JFK Had Ulcerative Colitis — Why You’re Not Alone
- Can Ayurvedic Medicine Help Ulcerative Colitis?
- Predicting Vedolizumab Response Early in IBD
- Learn about Biologicals used in UC and Crohn’s in Dubai
- IBD treatment update and advanced therapies
Ulcerative Colitis Diet, Lifestyle & Flare Control
- Ulcerative Colitis Diet: 3 Gut-Friendly Foods That Help Control Flares
- Can Coconut Oil Help with Ulcerative Colitis?
- Curcumin & Qing Dai in Ulcerative Colitis — What You Should Know
- Stress and Colitis — Why the Gut–Brain Connection Matters
Gut Microbiome, Leaky Gut & Overlooked Issues
- New Test for Diagnosing Crohn’s & Colitis: Microbiome-Based IBD Diagnosis
- Leaky Gut in IBD — What It Really Means
- IBD Breakthrough: How Gut Bacteria Unlock Natural Anti-Inflammatories
- SIBO in IBD — The Overlooked Issue You Shouldn't Ignore
Nutritional Deficiencies & Complications in IBD
Related Gastroenterology Topics
Digestive Conditions
- Gut Microbiome Test
- Irritable Bowel Syndrome (IBS)
- Crohn’s Disease
- Acid Reflux Treatment
- Gastritis
- H- Pylori Treatment
- Abdominal Pain
- Bloating
- Constipation
- Fatty Liver
- Rectal Bleeding
- Functional Dyspepsia
- Eosinophilic Esophagitis
- Food Intolerances
- Hemorrhoids
Diagnostic Tests & Procedures
- Hydrogen & Methane Breath Test (SIBO)
- Capsule Endoscopy
- Gastroscopy
- Colonoscopy
- CT Abdomen / CT Enterography
- MRI Abdomen / MR Enterography
- Urea Breath Test
- Fecal H. pylori Antigen
If you wish to discuss this further or would like to make an appointment, please use the booking form on this page. A member of our team will contact you within 12 business hours.
