By Dr Pranab Gyawali, Consultant Gastroenterologist
So let me explain clearly and scientifically.
What Is Leaky Gut?
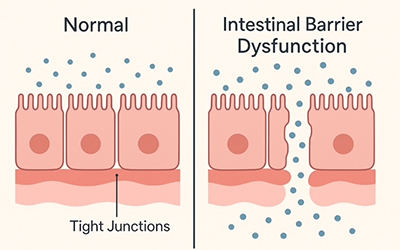
Leaky gut is a popular term, but in medical language, we refer to it as intestinal barrier dysfunction or increased intestinal permeability. This means the lining of the gut becomes weakened or damaged, allowing bacteria, toxins, or undigested food particles to “leak” into the bloodstream.
In a healthy gut, tight junction proteins keep the intestinal lining sealed. But in people with IBD, those tight junctions can be disrupted—leading to a cascade of inflammation, immune activation, and worsening symptoms.
How Leaky Gut Differs in Crohn’s vs. Ulcerative Colitis
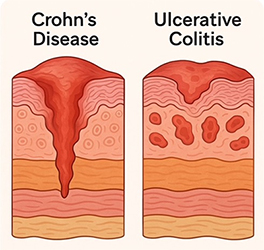
One of the most important things to understand is that leaky gut does not behave the same way in Crohn’s and UC.
Crohn’s Disease
In Crohn’s, intestinal barrier dysfunction can occur even before visible inflammation.
Studies have shown that relatives of Crohn’s patients can have increased gut permeability, suggesting that a “leaky gut” might play a role in triggering the disease.
The inflammation in Crohn’s is transmural—affecting all layers of the bowel wall—so barrier disruption can be deep and long-lasting.
Ulcerative Colitis
In UC, inflammation is typically limited to the mucosal layer (the surface of the colon).
Leaky gut in UC is usually a result of inflammation, not the cause.
However, during flares, the barrier can become severely compromised—and even during remission, subtle dysfunction may persist.
Why This Matters for Patients in Dubai
In my IBD clinic in Dubai, I see many patients who are overwhelmed by online advice and supplements promising to “fix” leaky gut. While there is some truth behind gut barrier dysfunction, it’s critical to separate science from hype.
What matters most is understanding:
- The mechanisms of barrier damage
- How they differ between Crohn’s and UC
- And how we can address them through real, evidence-based care
What Symptoms Might Suggest Barrier Dysfunction?
Even during IBD remission, you might still experience:
- Bloating or cramping
- Food sensitivities
- Fatigue or brain fog
- Skin issues or joint aches
These may not be due to active inflammation, but rather to a gut lining that’s still struggling to recover.
So What’s Next?
In Part 2 of this video series, I’ll explain:
How we can support the gut lining
What foods and microbiome strategies are backed by research
And which supplements might help—used in the right context
But most importantly, these strategies are meant to support—not replace—your medical treatment.
If you’re on medications like Imuran, Asacol, or biologics, don’t stop them. Supporting the gut barrier is an adjunct, not an alternative.
For all appointments and inquiries, please either WhatsApp +971 58 905 6211 or click here to request an appointment online.
