I’m Dr. Pranab Gyawali, a UK-trained Consultant Gastroenterologist practising in Dubai. Over the past 25 years, diarrhoea has been one of the most common symptoms I see — and in most patients, the cause is treatable once we understand what is driving it.
Many people think diarrhoea is always an infection, but the truth is that your gut has a few predictable ways of reacting when something irritates or overwhelms it. This page explains why diarrhoea happens, the specific causes I see in Dubai, and when it’s important to seek medical advice.
How Diarrhoea Actually Starts: The Gut’s Response
Your gut can produce diarrhoea in two main ways. Both are protective mechanisms, but when they become persistent, they need assessment.
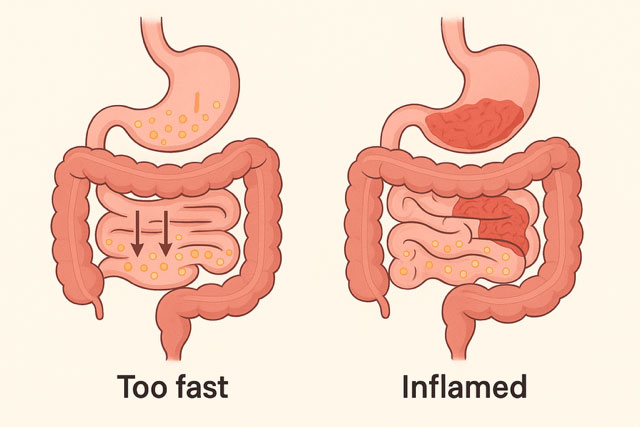
1. Everything Moves Too Fast (“rapid transit”)
Sometimes the intestines speed up to flush out something harmful — bacteria, toxins or food that did not agree with you. When food moves too quickly, the gut does not have time to absorb water, leading to loose, watery stools.
2. The Gut Lining Becomes Inflamed (poor absorption)
If the lining of the small intestine or colon becomes inflamed — from infection, Crohn’s disease, ulcerative colitis or post-infection sensitivity — it leaks fluid and loses its ability to absorb nutrients and water. This also produces diarrhoea, often with urgency, cramping or blood.
Common Causes of Diarrhoea in Dubai
Based on my clinical experience, these are the reasons I most often find in patients living in the UAE.
Acute (sudden) diarrhoea
These causes are very common in Dubai due to lifestyle and travel patterns:
- Foodborne infections (eating out, buffets, takeaway food)
- Viral gastroenteritis
- Travel-related bacteria (common for Dubai residents travelling to South Asia, East Africa and Europe)
- Sudden diet changes (new restaurants, rich foods, new cuisines)
- Stress-related diarrhoea / IBS flares
Longer-lasting or recurrent diarrhoea
These are the conditions I diagnose frequently in patients with ongoing or recurrent diarrhoea:
- Lactose intolerance (very common in Middle Eastern and Asian expat groups)
- Fructose intolerance (fruit juices, smoothies, desserts)
- IBS (irritable bowel syndrome) — especially IBS-D and mixed type
- Post-infectious gut sensitivity (ongoing diarrhoea after food poisoning)
- Crohn’s disease & ulcerative colitis
- Thyroid problems (overactive thyroid)
- Pancreatic enzyme insufficiency
- Bile acid diarrhoea, especially after gallbladder removal
- Medication-related diarrhoea (for example antibiotics, metformin, magnesium supplements)
When Diarrhoea Is No Longer “Protective”
If you have any of the following, a proper medical assessment is important:
- Diarrhoea lasting more than a few days
- Weight loss
- Waking up at night with diarrhoea
- Any blood in the stool
- Severe abdominal pain
- Fever
- Black or tarry stool
- Signs of dehydration (dry mouth, dizziness, dark urine)
- A known diagnosis of Crohn’s disease or ulcerative colitis and worsening symptoms
Persistent symptoms usually mean the gut is inflamed or unbalanced — and early evaluation makes a significant difference.
Symptoms of Diarrhoea
You may experience:
- Loose or watery stools
- Increased stool frequency
- Urgency to open bowels
- Bloating and cramps
- Nausea
- Sometimes fever or fatigue
- Dehydration (dry mouth, dizziness, dark urine)
How Diarrhoea Is Diagnosed
Your gastroenterologist may recommend some of the following tests:
- Stool tests — to check for infection, inflammation and parasites
- Faecal calprotectin — to help distinguish IBS from inflammatory bowel disease
- Blood tests — thyroid, coeliac screen and nutritional deficiencies
- Lactose or fructose breath tests
- SIBO test (hydrogen/methane breath test)
- Colonoscopy if there are red flags or inflammatory bowel disease is suspected
- Ultrasound or CT scan if needed, based on your symptoms and examination
The aim is always the same: to understand why it is happening, so that treatment can be targeted and effective.
Treatment of Diarrhoea
Treatment depends entirely on the underlying cause:
- Rehydration and electrolytes to correct fluid loss
- Short-term dietary adjustments (lighter, low-fibre foods initially)
- Treating infections when confirmed
- Removing dietary triggers such as lactose or fructose
- Managing IBS-D with diet, gut-directed therapies and, when appropriate, medication
- Controlling gut inflammation in Crohn’s disease or ulcerative colitis
- Enzyme replacement for pancreatic insufficiency
- Bile-acid binders for bile acid diarrhoea
For most people, diarrhoea improves significantly once the underlying cause is identified and addressed.
Common Patient Questions — Answered by Dr. Pranab
Q1. How do I treat food poisoning diarrhoea in Dubai?
Start with hydration (water plus electrolytes) and simple, low-fibre foods for 24–48 hours. If there is fever, blood in the stool, severe pain or symptoms lasting more than a few days, it is no longer something to self-manage at home — you should seek medical assessment to rule out infection or inflammation.
Q2. What is the difference between chronic diarrhoea, IBS and IBD?
IBS-D causes diarrhoea because the gut is sensitive and moves too fast, but there is no visible inflammation on tests or colonoscopy. Inflammatory bowel disease (such as Crohn’s disease and ulcerative colitis) involves true inflammation of the gut lining and often causes blood in the stool, weight loss or waking at night with urgency. Chronic diarrhoea simply means diarrhoea lasting longer than four weeks — the specialist’s role is to find out which problem is responsible.
Q3. Can stress and anxiety cause diarrhoea or IBS in Dubai?
Yes. Dubai is a fast-paced, high-pressure environment and the brain–gut connection means that stress and anxiety can speed up the intestines, trigger IBS-D and worsen post-infectious gut sensitivity. Looking after both your gut and your stress levels is often important for long-term control.
Q4. When should I stop self-treating and see a gastroenterologist?
If your diarrhoea is persistent, waking you at night, causing weight loss or there is any blood in the stool, your gut is giving you a warning that needs specialist assessment. Other red flags include fever, black or tarry stools, severe abdominal pain and signs of dehydration.
Internal Resources & Related Topics
- Crohn’s disease — diagnosis and treatment in Dubai
- Ulcerative colitis — flares, management and follow-up
- IBS (Irritable Bowel Syndrome) — IBS-D, IBS-M and gut sensitivity
- Hydrogen & Methane Breath Test (SIBO) in Dubai
- How often should you poop? — what is normal
- Brain–Gut Connection — how stress affects your gut
